29 results
Regional impact of multidrug-resistant organism prevention bundles implemented by facility type: A modeling study
- Samuel E. Cincotta, Maroya S. Walters, D. Cal Ham, Rany Octaria, Jessica M. Healy, Rachel B. Slayton, Prabasaj Paul
-
- Journal:
- Infection Control & Hospital Epidemiology , First View
- Published online by Cambridge University Press:
- 28 February 2024, pp. 1-8
-
- Article
- Export citation
-
Background:
Emerging multidrug-resistant organisms (MDROs), such as carbapenem-resistant Enterobacterales (CRE), can spread rapidly in a region. Facilities that care for high-acuity patients with longer stays may have a disproportionate impact on this spread.
Objective:We assessed the impact of implementing preventive interventions, directed at a subset of facilities, on regional prevalence.
Methods:We developed a deterministic compartmental model, parametrized using CRE and patient transfer data. The model included the community and healthcare facilities within a US state. Individuals may be either susceptible or infectious with CRE. Individuals determined to be infectious through admission screening, periodic prevalence surveys (PPSs), or interfacility communication were placed in a state of lower transmissibility if enhanced infection prevention and control (IPC) practices were in place at a facility.
Results:Intervention bundles that included PPS and enhanced IPC practices at ventilator-capable skilled nursing facilities (vSNFs) and long-term acute-care hospitals (LTACHs) had the greatest impact on regional prevalence. The benefits of including targeted admission screening in acute-care hospitals, LTACHs, and vSNFs, and improved interfacility communication were more modest. Daily transmissions in each facility type were reduced following the implementation of interventions primarily focused at LTACHs and vSNFs.
Conclusions:Our model suggests that interventions that include screening to limit unrecognized MDRO introduction to, or dispersal from, LTACHs and vSNFs slow regional spread. Interventions that pair detection and enhanced IPC practices within LTACHs and vSNFs may substantially reduce the regional burden.
Concurrent transmission of multiple carbapenemases in a long-term acute-care hospital
- Danielle A. Rankin, Maroya Spalding Walters, Luz Caicedo, Paige Gable, Heather A. Moulton-Meissner, Allison Chan, Albert Burks, Kendra Edwards, Gillian McAllister, Alyssa Kent, Alison Laufer Halpin, Christina Moore, Tracy McLemore, Linda Thomas, Nychie Q. Dotson, Alvina K. Chu
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 45 / Issue 3 / March 2024
- Published online by Cambridge University Press:
- 10 January 2024, pp. 292-301
- Print publication:
- March 2024
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Objective:
We investigated concurrent outbreaks of Pseudomonas aeruginosa carrying blaVIM (VIM-CRPA) and Enterobacterales carrying blaKPC (KPC-CRE) at a long-term acute-care hospital (LTACH A).
Methods:We defined an incident case as the first detection of blaKPC or blaVIM from a patient’s clinical cultures or colonization screening test. We reviewed medical records and performed infection control assessments, colonization screening, environmental sampling, and molecular characterization of carbapenemase-producing organisms from clinical and environmental sources by pulsed-field gel electrophoresis (PFGE) and whole-genome sequencing.
Results:From July 2017 to December 2018, 76 incident cases were identified from 69 case patients: 51 had blaKPC, 11 had blaVIM, and 7 had blaVIM and blaKPC. Also, blaKPC were identified from 7 Enterobacterales, and all blaVIM were P. aeruginosa. We observed gaps in hand hygiene, and we recovered KPC-CRE and VIM-CRPA from drains and toilets. We identified 4 KPC alleles and 2 VIM alleles; 2 KPC alleles were located on plasmids that were identified across multiple Enterobacterales and in both clinical and environmental isolates.
Conclusions:Our response to a single patient colonized with VIM-CRPA and KPC-CRE identified concurrent CPO outbreaks at LTACH A. Epidemiologic and genomic investigations indicated that the observed diversity was due to a combination of multiple introductions of VIM-CRPA and KPC-CRE and to the transfer of carbapenemase genes across different bacteria species and strains. Improved infection control, including interventions that minimized potential spread from wastewater premise plumbing, stopped transmission.
Colonization screening positivity rates for novel multidrug-resistant organism healthcare containment responses during 2019–2022
- Danielle Rankin, Lucas Ochoa, Guillermo Sanchez, Kaitlin Forsberg, Meghan Lyman, Nijika Shrivastwa, Maroya Walters
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s101-s102
-
- Article
-
- You have access Access
- Open access
- Export citation
-
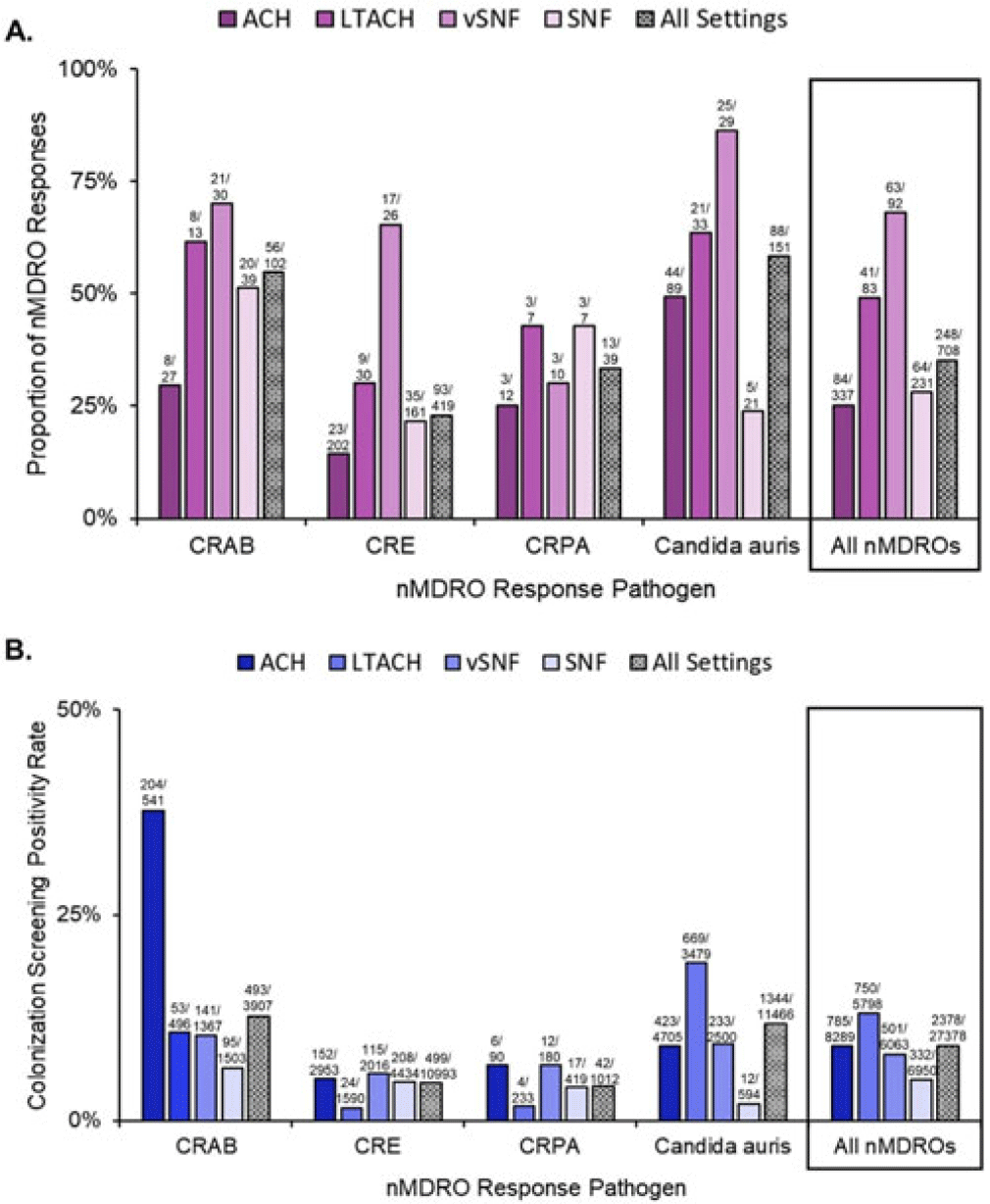
Background: The CDC recommends a public health response when novel and targeted multidrug-resistant organisms (nMDROs), such as carbapenem-resistant organisms or Candida auris, are identified in healthcare settings in nonendemic areas. nMDRO responses are supported by healthcare-associated infection-antimicrobial resistance programs in 50 state and 6 local and territorial health departments. Annually, health departments report nMDRO responses to the CDC. We summarize nMDRO responses nationally and report our assessment of colonization screening positivity rates by healthcare setting and pathogen. Methods: We analyzed nMDRO response data reported by health departments for the period August 2019–July 2021; we excluded prevention efforts (ie, widespread screening based on facility-level risk factors). Among nMDRO responses in which colonization screening was performed, we calculated the proportion of responses in which screening detected additional cases of the index nMDRO and the colonization screening positivity, by healthcare setting and pathogen. Results: Among 2,051 nMDRO responses, 732 (36%) had ≥1 colonization screening (representing 44,845 colonization screenings), of which 24 (representing 17,467 colonization screenings) were prevention efforts and were excluded. Among the remaining 708 nMDRO responses, the healthcare setting most frequently included was acute-care hospitals (ACHs; 337 of 708, 48%); the least frequently included was long-term ACHs (LTACHs; 83 of 708, 12%). Carbapenem-resistant Enterobacterales were the most common index nMDRO prompting a response (408 of 708, 58%). Screening identified additional cases of the index nMDRO in 248 responses (35%) and 2,378 (9%) of 27,378 colonization screenings. Identification of the index nMDRO varied by pathogen and setting (Fig. 1). Overall, ventilator-capable skilled nursing facilities (vSNFs) were the facility type in which colonization screening most frequently identified additional cases of the index nMDRO (63 of 92 responses, 63%), and LTACHs had the highest colonization screening positivity (750 of 5,798, 13%). Similar colonization screening positivity was observed in ACHs (9%) and vSNFs (8%). On average, Candida auris and carbapenem-resistant Acinetobacter baumannii (CRAB) had the highest colonization screening positivity rates across all healthcare settings: CRAB, 493 (12.6%) of 3,907 screened; Candida auris, 1,344 (11.7%) of 11,466 screened (Fig. 1B). More than one-half of responses identified ≥1 case of the index nMDRO. Conclusions: During public health nMDRO responses, additional cases were regularly identified through colonization screening. Responses in vSNFs and LTACHs and to environmental pathogens like Candida auris and CRAB detected additional cases in more than one-half of responses, suggesting that spread commonly occurred prior to detection of the first clinical case. The use of colonization screening is an effective strategy to detect unidentified nMDRO colonization, especially in high-acuity postacute-care settings.
Disclosures: None
New Delhi metallo-β-lactamase–producing Escherichia coli among dogs at an animal rescue facility—Wisconsin, 2022
- Kiara McNamara, Caroline Habrun, W. Wyatt Wilson, Leslie Kollmann, G. Sean Stapleton, Richard Stanton, Katharine Benedict, Amanda Beaudoin, Paula Snippes, Melissa Anacker, Megin Nichols, Maroya Walters, Jordan Mason, Nikki Mueller
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, p. s90
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: New Delhi Metallo-β-lactamase (NDM)–producing Escherichia coli are highly resistant organisms that spread quickly. In the United States, organisms with blaNDM are rare and mostly associated with healthcare settings. However, in other countries, blaNDM can be relatively common and are found in community settings. State veterinary and public health partners detected NDM E. coli in a dog from Iran living at a Wisconsin animal rescue facility (ARF), where 40% of dogs had international origins. We investigated to determine spread among dog and human contacts and prevent further transmission. Methods: We screened dogs and humans at the ARF, a local veterinary clinic (clinic A), and ARF staff homes (homes A and B) for colonization with blaNDM. We reviewed veterinary records and conducted a case–control analysis to identify risk factors for blaNDM acquisition among dogs. We evaluated ARF infection control practices. Screening specimens that were positive for blaNDM were cultured. We conducted an analysis of short- and long-read whole-genome sequencing data to evaluate isolate relatedness. We compared NDM E. coli sequences from dogs to all NDM E. coli sequences from humans collected in Wisconsin and nearby states. Results: Screening identified blaNDM colonization in 27 (37%) of 73 ARF dogs and 4 (56%) of 7 dogs in home A, but not in ARF or staff in clinic A. Among ARF dogs with blaNDM, 20 (74%) 27 had international origins and 22 (81%) had ≥1 medical condition. Dogs sharing the same space (OR, 5.1; 95% CI, 1.8–14.7) were associated with blaNDM acquisition. We observed high animal density, soiled environments, and insufficient hand hygiene. ARF staff wore workwear and work shoes off site, including to home A. Sequencing identified 3 multilocus sequence types (STs) using the Achtman scheme among 27 isolates with blaNDM-5. Most isolates were ST361 (20 of 27, 74%) followed by ST167 (6 of 27, 22%) and ST1163 (1 of 27, 4%). Within-MLST cluster variability was <1–3 high-quality single-nucleotide variant differences, each harboring a ST-specific plasmid with blaNDM-5. No NDM-E. coli sequences from humans appeared related. Conclusions: Investigation of a single isolate led to identification of widespread NDM-E. coli transmission among dogs at an ARF. There were multiple NDM E. coli introductions to the ARF, likely by dogs of international origin. Poor hygiene contributed to transmission among ARF dogs and to dogs outside the ARF. Transmission of blaNDM-5 at the ARF and offsite spread to home A demonstrate the potential for unrecognized community sources to disseminate NDM E. coli in community settings. Strategies and lessons learned from interventions to prevent antibiotic resistance in human healthcare settings may inform and support prevention in animal care.
Disclosures: None
An interactive patient transfer network and model visualization tool for multidrug-resistant organism prevention strategies
- Rany Octaria, Samuel Cincotta, Jessica Healy, Camden Gowler, Prabasaj Paul, Maroya Walters, Rachel Slayton
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s120-s122
-
- Article
-
- You have access Access
- Open access
- Export citation
-
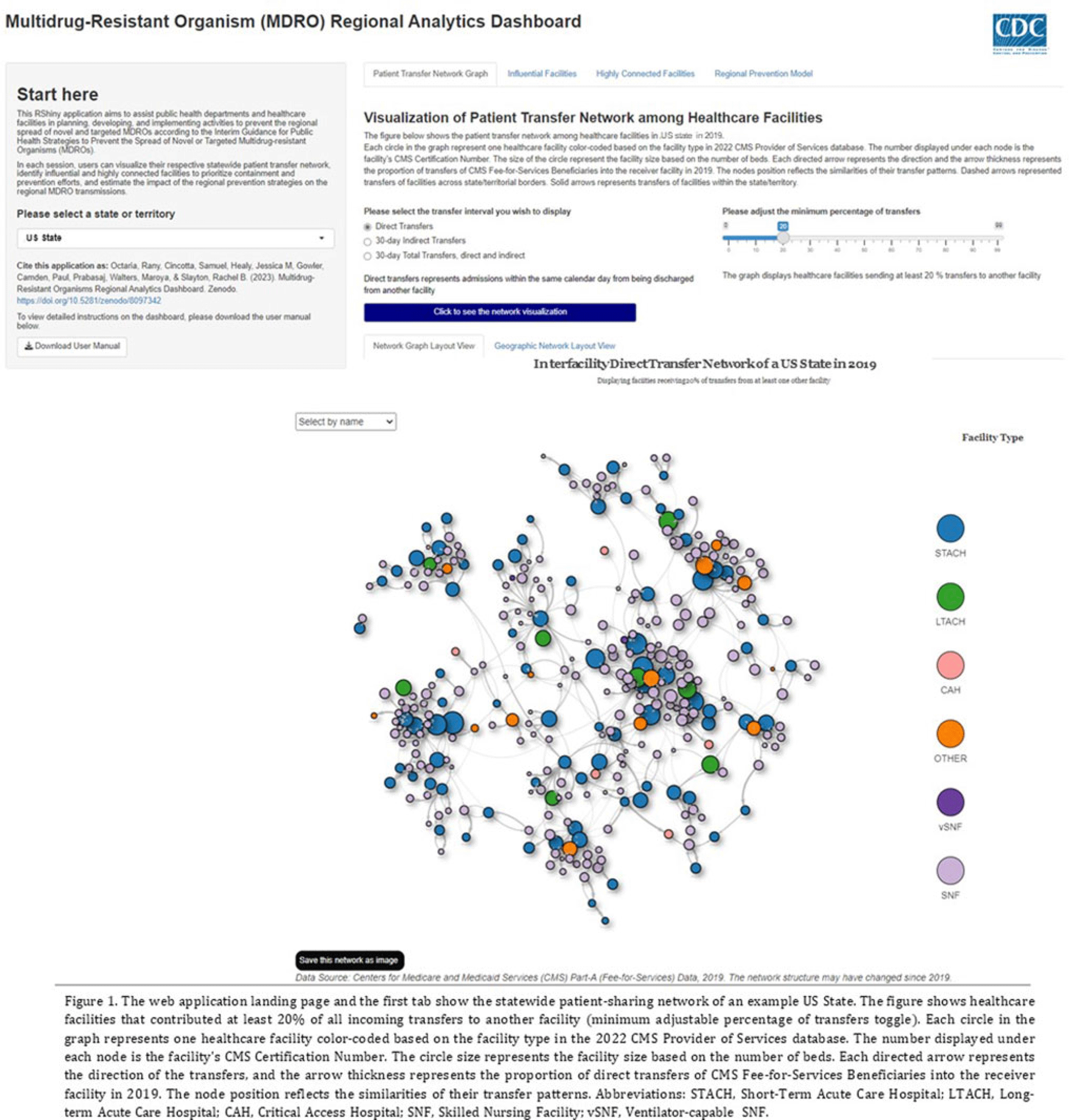
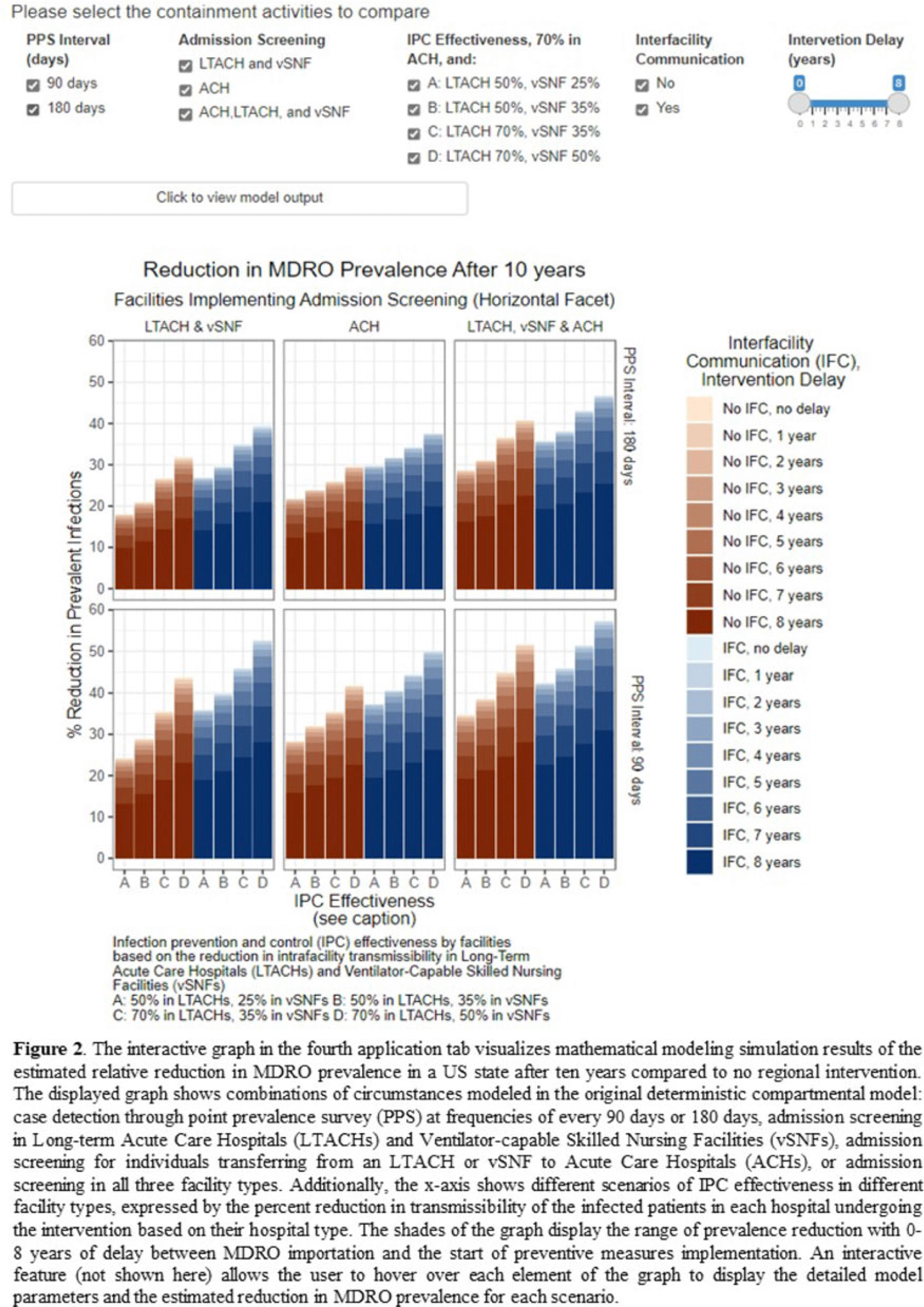
Background: The CDC’s new Public Health Strategies to Prevent the Spread of Novel and Targeted Multidrug-Resistant Organisms (MDROs) were informed by mathematical models that assessed the impact of implementing preventive strategies directed at a subset of healthcare facilities characterized as influential or highly connected based on their predicted role in the regional spread of MDROs. We developed an interactive tool to communicate mathematical modeling results and visualize the regional patient transfer network for public health departments and healthcare facilities to assist in planning and implementing prevention strategies. Methods: An interactive RShiny application is currently hosted in the CDC network and is accessible to external partners through the Secure Access Management Services (SAMS). Patient transfer volumes (direct and indirect, that is, with up to 30 days in the community between admissions) were estimated from the CMS fee-for-service claims data from 2019. The spread of a carbapenem-resistant Enterobacterales (CRE)–like MDROs within a US state was simulated using a deterministic model with susceptible and infectious compartments in the community and healthcare facilities interconnected through patient transfers. Individuals determined to be infectious through admission screening, point-prevalence surveys (PPSs), or notified from interfacility communication were assigned lower transmissibility if enhanced infection prevention and control practices were in place at a facility. Results: The application consists of 4 interactive tabs. Users can visualize the statewide patient-sharing network for any US state and select territories in the first tab (Fig. 1). A feature allows users to highlight a facility of interest and display downstream or upstream facilities that received or sent transfers from the facility of interest, respectively. A second tab lists influential facilities to aid in prioritizing screening and prevention activities. A third tab lists all facilities in the state in descending order of their dispersal rate (ie, the rate at which patients are shared downstream to other facilities), which can help identify highly connected facilities. In the fourth tab, an interactive graph displays the predicted reduction of MDRO prevalence given a range of intervention scenarios (Fig. 2). Conclusions: Our RShiny application, which can be accessed by public health partners, can assist healthcare facilities and public health departments in planning and tailoring MDRO prevention activity bundles.
Disclosures: None
Investigation of the first cluster of Candida auris cases among pediatric patients in the United States―Nevada, May 2022
- Sophie Jones, Kaitlin Forsberg, Christopher Preste, Joe Sexton, Paige Gable, Janet Glowicz, Heather Jones, Maroya Walters, Meghan Lyman, Chidinma Njoku, Kimisha Causey, Jeanne Ruff, Dallas Smith, Karen Wu, Elizabeth Misas, Teri Lynn, Chantal Lewis, Brian Min, Fathia Osman, Erin Archer
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s118-s119
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Candida auris is a frequently drug-resistant yeast that can cause invasive disease and is easily transmitted in healthcare settings. Pediatric cases are rare in the United States, with <10 reported before 2022. In August 2021, the first C. auris case in Las Vegas was identified in an adult. By May 2022, 117 cases were identified across 16 healthcare facilities, including 3 pediatric cases at an acute-care hospital (ACH) with adult cases, representing the first pediatric cluster in the United States. The CDC and Nevada Division of Public and Behavioral Health (NVDPBH) sought to describe these cases and risk factors for C. auris acquisition. Methods: We defined a case as a patient’s first positive C. auris specimen. We reviewed medical records and infection prevention and control (IPC) practices. Environmental sampling was conducted on high-touch surfaces throughout affected adult and pediatric units. Isolate relatedness was assessed using whole-genome sequencing (WGS). Results: All 3 pediatric patients were born at the facility and had congenital heart defects. All were aged <6 months when they developed C. auris bloodstream infections; 2 developed C. auris endocarditis. One patient died. Patients overlapped in the pediatric cardiac intensive care unit; 2 did not leave between birth and C. auris infection. Mobile medical equipment was shared between adult and pediatric patients; lapses in cleaning and disinfection of shared mobile medical equipment and environmental surfaces were observed, presenting opportunities for transmission. Overall, 32 environmental samples were collected, and C. auris was isolated from 2 specimens from an adult unit without current cases. One was a composite sample from an adult patient’s bed handles, railings, tray table and call buttons, and the second was from an adult lift-assistance device. WGS of specimens from adult and pediatric cases and environmental isolates were in the same genetic cluster, with 2–10 single-nucleotide polymorphisms (SNPs) different, supporting within-hospital transmission. The pediatric cases varied by 0–3 SNPs; at least 2 were highly related. Conclusions: C. auris was likely introduced to the pediatric population from adults via inadequately cleaned and disinfected mobile medical equipment. We made recommendations to ensure adequate cleaning and disinfection and implement monitoring and audits. No pediatric cases have been identified since. This investigation demonstrates transmission can occur between unrelated units and populations and that robust infection prevention and control practices throughout the facility are critical for reducing C. auris environmental burden and limiting transmission, including to previously unaffected vulnerable populations, like children.
Disclosures: None
Outbreak response activities conducted by public health programs in healthcare facilities nationwide, August 2019–July 2020
- Nijika Shrivastwa, Lucas Ochoa, Maroya Walters, Kiran Perkins, Joseph Perz, Jennifer C. Hunter
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, p. s15
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Rapid response is critical to control healthcare-associated infection (HAI) and antibiotic resistance threats within healthcare facilities to prevent illness among patients, residents, and healthcare personnel. Through this analysis, we aimed to quantify public health response activities, by healthcare setting type, for (1) novel and targeted multidrug-resistant organisms or mechanisms (MDROs), (2) SARS-CoV-2, and (3) other possible outbreaks. Method: We reviewed response activity data submitted by US state, territorial, and local health department HAI/AR programs to the CDC as part of funding requirements. We performed descriptive analyses of response activities conducted during the funding reporting period (August 2019–July 2020). SARS-CoV-2 response activities were reported from January through July 2020. Data were analyzed by response category (novel or targeted MDRO, SARS-CoV-2, other HAI/AR responses), and healthcare setting type. Results: During August 2019–July 2020, 57 HAI/AR Programs (50 state, 1 territorial, 5 local health departments, and District of Columbia) reported 18,306 public health responses involving healthcare facilities. These data included 3,860 responses to 1 or more cases of novel or targeted MDROs, 13,992 responses to SARS-CoV-2 outbreaks (beginning in January 2020), and 454 responses to other possible outbreaks. Novel and targeted MDRO responses most frequently occurred in acute-care hospitals (ACHs, 64.5%), skilled nursing facilities (SNFs, 24.5%), and long-term acute-care hospitals (LTACHs, 5.8%). SARS-CoV-2 responses most frequently occurred in SNFs (55%), and assisted living facilities (24%). Other HAI/AR responses most frequently occurred in ACH (50%), SNF (28.4%), and outpatient settings (19.6%). Of the “other” HAI/AR responses, 76% were responses to cases, clusters, or outbreaks, and 23.8% were responses to serious infection control breaches including device and instrument reprocessing, injection safety, and other deficient practices. Conclusions: During the study period, public health programs performed a high volume of HAI/AR response activities largely focused on SARS-CoV-2 in nursing homes and assisted living facilities. Other important response activities occurred across a range of other healthcare settings, including responses to novel and targeted MDROs, HAI outbreaks, and serious infection control breaches. Whereas SARS-CoV-2 response activities largely centered in long-term care settings, MDRO and other HAI/AR responses occurred mostly in acute-care settings. These data demonstrate the importance of building and sustaining public health response capacity for a broad array of healthcare settings, pathogens, and patient populations to meet the range of current and emerging HAI/AR threats.
Funding: None
Disclosures: None
Predicting the regional impact of interventions to prevent and contain multidrug-resistant organisms
- Samuel Cincotta, Elizabeth Soda, Rachel Slayton, David Ham, Maroya Walters, Prabasaj Paul
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, pp. s13-s14
-
- Article
-
- You have access Access
- Open access
- Export citation
-
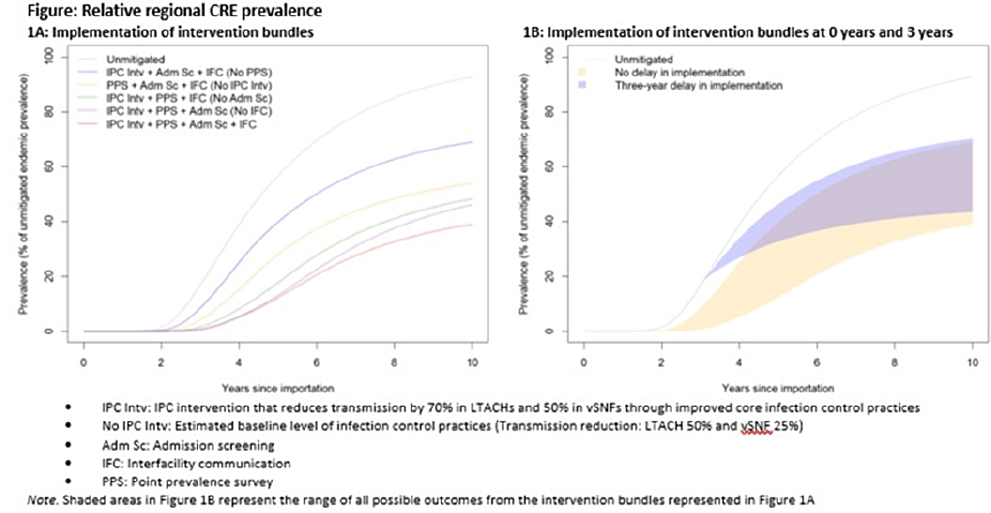
Background: Multidrug-resistant organisms (MDROs), such as carbapenem-resistant Enterobacterales (CRE), can spread rapidly in a region. Facilities that care for high-acuity patients with long average lengths of stay (eg, long-term acute-care hospitals or LTACHs and ventilator-capable skilled nursing facilities or vSNFs) may amplify this spread. We assessed the impact of interventions on CRE spread within a region individually, bundled, and implemented at different facility types. Methods: We developed a deterministic compartmental model, parametrized using CRE data reported to the NHSN and patient transfer data from the CMS specific to a US state. The model includes the community and the healthcare facilities within the state. Individuals may be either susceptible or infected and infectious. Infected patients determined to have CRE through admission screening or point-prevalence surveys at a facility are placed in a state of lower transmissibility if enhanced infection prevention and control (IPC) practices are in place. Results: Intervention bundles that included periodic point-prevalence surveys and enhanced IPC at high-acuity postacute-care facilities had the greatest impact on regional prevalence 10 years into an outbreak; the benefits of including admission screening and improved interfacility communication were more modest (Fig. 1A). Delaying interventions by 3 years is predicted to result in smaller reductions in prevalence (Fig. 1B). Increasing the frequency of point-prevalence surveys from biannually to quarterly resulted in a substantial relative reduction in prevalence (from 25% to 44%) if conducted from the start of an outbreak. IPC improvements in vSNFs resulted in greater relative reductions than in LTACHs. Admission screening at LTACHs and vSNFs was predicted to have a greater impact on prevalence if in place prior to CRE introduction (~20% reduction), and the impact decreased by approximately half if implementation was delayed until 3 years after CRE introduction. In contrast, the effect of admission screening in ACH was less (~10% reduction in prevalence) and did not change with implementation delays. Conclusions: Our model suggests that interventions that limit unrecognized MDRO introduction to, or dispersal from, LTACHs and vSNFs through screening are predicted to slow distribution regionally. Interventions to detect colonization and improve IPC practices within LTACHs and vSNFs may substantially reduce the regional burden. Prevention strategies are predicted to have the greatest impact when interventions are bundled and implemented before an MDRO is identified in a region, but reduction in overall prevalence is still possible if implemented after initial MDRO spread.
Funding: None
Disclosures: None
Trimethoprim-sulfamethoxazole resistance patterns among Staphylococcus aureus in the United States, 2012–2018
- D. Cal Ham, Lucy Fike, Hannah Wolford, Lindsey Lastinger, Minn Soe, James Baggs, Maroya Spalding Walters
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 5 / May 2023
- Published online by Cambridge University Press:
- 15 February 2022, pp. 794-797
- Print publication:
- May 2023
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
We reviewed trimethoprim-sulfamethoxazole antibiotic susceptibility testing data among Staphylococcus aureus using 3 national inpatient databases. In all 3 databases, we observed an increases in the percentage of methicillin-resistant Staphylococcus aureus that were not susceptible to trimethoprim-sulfamethoxazole. Providers should select antibiotic regimens based on local resistance patterns and should report changes to the public health department.
Verona Integron-Encoded Metallo-Beta-Lactamase (VIM)–Producing Pseudomonas aeruginosa Outbreak Associated with Acute Care
- Allison Chan, Alicia Shugart, Albert Burks, Christina Moore, Paige Gable, Heather Moulton-Meissner, Gillian McAllister, Alison Halpin, Maroya Walters, Amelia Keaton, Kelley Tobey, Katie Thure, Sarah Schmedes, Paige Gable, Henrietta Hardin, Adrian Lawsin
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, p. s26
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Contaminated healthcare facility plumbing is increasingly recognized as a source of carbapenemase-producing organisms (CPOs). In August 2019, the Tennessee State Public Health Laboratory identified Tennessee’s twelfth VIM-producing carbapenem-resistant Pseudomonas aeruginosa (VIM-CRPA), from a patient in a long-term acute-care hospital. To determine a potential reservoir, the Tennessee Department of Health (TDH) reviewed healthcare exposures for all cases. Four cases (33%), including the most recent case and earliest from March 2018, had a history of admission to intensive care unit (ICU) room X at acute-care hospital A (ACH A), but the specimens were collected at other facilities. The Public Health Laboratory collaborated with ACH A to assess exposures, perform environmental sampling, and implement control measures. Methods: TDH conducted in-person infection prevention assessments with ACH A, including a review of the water management program. Initial recommendations included placing all patients admitted to room X on contact precautions, screening for CPO on room discharge, daily sink basin and counter cleaning, and other sink hygiene measures. TDH collected environmental and water samples from 5 ICU sinks (ie, the handwashing and bathroom sinks in room X and neighboring room Y [control] and 1 hallway sink) and assessed the presence of VIM-CRPA. Moreover, 5 patients and 4 environmental VIM-CRPA underwent whole-genome sequencing (WGS). Results: From February to June 2020, of 21 patients admitted to room X, 9 (43%) underwent discharge screening and 4 (44%) were colonized with VIM-CRPA. Average room X length of stay was longer for colonized patients (11.3 vs 4.8 days). Drain swabs from room X’s bathroom and handwashing sinks grew VIM-CRPA; VIM-CRPA was not detected in tap water or other swab samples. VIM-CRPA from the environment and patients were sequence type 253 and varied by 0–13 single-nucleotide variants. ACH A replaced room X’s sinks and external plumbing in July. Discharge screening and contact precautions for all patients were discontinued in November, 5 months following the last case and 12 consecutive negative patient discharge screens. Improved sink hygiene and mechanism testing for CRPA from clinical cultures continued, with no new cases identified. Conclusions: An ICU room with a persistently contaminated sink drain was a persistent reservoir of VIM-CRPA. The room X attack rate was high, with VIM-CRPA acquisition occurring in >40% of patients screened. The use of contaminated plumbing fixtures in ACH have the potential to facilitate transmission to patients but may be challenging to identify and remediate. All healthcare facilities should follow sink hygiene best practices.
Funding: No
Disclosures: None
Aggressive Colonization Screening and Infection Control Measures in Containment of NDM-5 Carbapenemase-Producing CRE
- Ishrat Kamal-Ahmed, Kate Tyner, Teresa Fitzgerald, Heather Adele Moulton-Meissner, Gillian McAllister, Alison Halpin, Muhammad Salman Ashraf, Tom Safranek, Maroya Walters, Maureen Tierney
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s458-s459
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: In April 2019, Nebraska Public Health Laboratory identified an NDM-producing Enterobacter cloacae from a urine sample from a rehabilitation inpatient who had recently received care in a specialized unit (unit A) of an acute-care hospital (ACH-A). After additional infections occurred at ACH-A, we conducted a public health investigation to contain spread. Methods: A case was defined as isolation of NDM-producing carbapenem-resistant Enterobacteriaceae (CRE) from a patient with history of admission to ACH-A in 2019. We conducted clinical culture surveillance, and we offered colonization screening for carbapenemase-producing organisms to all patients admitted to unit A since February 2019. We assessed healthcare facility infection control practices in ACH-A and epidemiologically linked facilities by visits from the ICAP (Infection Control Assessment and Promotion) Program. The recent medical histories of case patients were reviewed. Isolates were evaluated by whole-genome sequencing (WGS). Results: Through June 2019, 7 cases were identified from 6 case patients: 4 from clinical cultures and 3 from 258 colonization screens including 1 prior unit A patient detected as an outpatient (Fig. 1). Organisms isolated were Klebsiella pneumoniae (n = 5), E. cloacae (n = 1), and Citrobacter freundii (n = 1); 1 patient had both NDM-producing K. pneumoniae and C. freundii. Also, 5 case patients had overlapping stays in unit A during February–May 2019 (Fig. 2); common exposures in unit A included rooms in close proximity, inhabiting the same room at different times and shared caregivers. One case-patient was not admitted to unit A but shared caregivers, equipment, and devices (including a colonoscope) with other case patients while admitted to other ACH-A units. No case patients reported travel outside the United States. Screening at epidemiologically linked facilities and clinical culture surveillance showed no evidence of transmission beyond ACH-A. Infection control assessments at ACH-A revealed deficiencies in hand hygiene, contact precautions adherence, and incomplete cleaning of shared equipment within and used to transport to/from a treatment room in unit A. Following implementation of recommended infection control interventions, no further cases were identified. Finally, 5 K. pneumoniae of ST-273 were related by WGS including carriage of NDM-5 and IncX3 plasmid supporting transmission of this strain. Further analysis is required to relate IncX3 plasmid carriage and potential transmission to other organisms and sequence types identified in this study. Conclusions: We identified a multiorganism outbreak of NDM-5–producing CRE in an ACH specialty care unit. Transmission was controlled through improved infection control practices and extensive colonization screening to identify asymptomatic case-patients. Multiple species with NDM-5 were identified, highlighting the potential role of genotype-based surveillance.
Funding: None
Disclosures: Muhammad Salman Ashraf reports that he is the principal investigator for a study funded by an investigator-initiated research grant.
Carbapenemase-Producing, Carbapenem-Resistant Acinetobacter baumannii: Summary of CDC Consultations, 2017–2019
- Lauren Epstein, Alicia Shugart, David Ham, Snigdha Vallabhaneni, Richard Brooks, Gillian McAllister, Alison Halpin, Sarah Gilbert, Maroya Walters
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s151-s152
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Carbapenemase-producing carbapenem-resistant Acinetobacter baumannii (CP-CRAB) are a public health threat due to potential for widespread dissemination and limited treatment options. We describe CDC consultations for CP-CRAB to better understand transmission and identify prevention opportunities. Methods: We defined CP-CRAB as CRAB isolates with a molecular test detecting KPC, NDM, VIM, or IMP carbapenemases or a plasmid-mediated oxacillinase (OXA-23, OXA-24/40, OXA-48, OXA-58, OXA-235/237). We reviewed the CDC database of CP-CRAB consultations with health departments from January 1, 2017, through June 1, 2019. Consultations were grouped into 3 categories: multifacility clusters, single-facility clusters, and single cases. We reviewed the size, setting, environmental culturing results, and identified infection control gaps for each consultation. Results: We identified 29 consultations involving 294 patients across 19 states. Among 9 multifacility clusters, the median number of patients was 12 (range, 2–87) and the median number of facilities was 2 (range, 2–6). Among 9 single-facility clusters, the median number of patients was 5 (range, 2–50). The most common carbapenemase was OXA-23 (Table 1). Moreover, 16 consultations involved short-stay acute-care hospitals, and 6 clusters involved ICUs and/or burn units. Also, 8 consultations involved skilled nursing facilities. Environmental sampling was performed in 3 consultations; CP-CRAB was recovered from surfaces of portable, shared equipment (3 consultations), inside patient rooms (3 consultations) and nursing stations (2 consultations). Lapses in environmental cleaning and interfacility communication were common across consultations. Among 11 consultations for single CP-CRAB cases, contact screening was performed in 7 consultations and no additional CP-CRAB was identified. All 4 patients with NDM-producing CRAB reported recent international travel. Conclusions: Consultations for clusters of oxacillinase-producing CP-CRAB were most often requested in hospitals and skilled nursing facilities. Healthcare facilities and public health authorities should be vigilant for possible spread of CP-CRAB via shared equipment and the potential for CP-CRAB spread to connected healthcare facilities.
Funding: None
Disclosures: None
Changing US Epidemiology of NDM-Producing Carbapenem-Resistant Enterobacteriaceae, 2017–2019
- Alicia Shugart, Garrett Mahon, Lauren Epstein, Jennifer Y. Huang, Gillian McAllister, Adrian Lawsin, Erisa Sula, Alison Laufer Halpin, Amanda Smith, Rebekah Carman, P. Maureen Cassidy, Karim Morey, Anu Paranandi, Randy Downing, Diane Noel, , Alexander J. Kallen, Maroya Spalding Walters
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s25-s26
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Due to limited therapeutic options and potential for spread, carbapenem-resistant Enterobacteriaceae (CRE)-producing New Delhi metallo-β-lactamases (NDMs) are a public health priority. We investigated the epidemiology of NDM-producing CRE reported to the CDC to clarify its distribution and relative prevalence. Methods: The CDC’s Antibiotic Resistance Laboratory Network supports molecular testing of CRE for 5 carbapenemases nationally. Although KPC is the most common carbapenemase in the United States, non-KPC carbapenemases are a growing concern. We analyzed CRE with any of 4 non-KPC plasmid-mediated carbapenemases (NDM, VIM, IMP, or OXA-48 type) isolated from specimens collected from January 1, 2017, through June 30, 2019; only a patient’s first isolate per organism–carbapenemase combination was included. We excluded isolates from specimen sources associated with colonization screening (eg, perirectal). We compared the proportion of NDM-producing CRE to all non-KPC–producing CP-CRE between period A (January to June 2018) and period B (January to June 2019). Health departments and the CDC collected additional exposure and molecular information in selected states to better describe current NDM-producing CRE epidemiology. Results: Overall, 47 states reported 1,013 non–KPC-producing CP-CRE (range/state, 1–109 isolates; median, 11 isolates); 46 states reported 631 NDM-producing CRE (range/state, 1–84; median, 6). NDM-producing CRE increased quarterly from the third quarter of 2018 through the second quarter of 2019; CP-CRE isolates with other non-KPC carbapenemases remained stable (Fig. 1). In period A, 124 of 216 emerging CP-CRE had NDM (57.1%), compared with 255 of 359 emerging CP-CRE (71.0%) during period B (P = .1179). Among NDM-producing CRE, the proportion of Enterobacter spp increased from 10.5% in 2018 to 18.4% in 2019 (P = .0467) (Fig. 2). In total, 18 states reported more NDM-producing CRE in the first 6 months of 2019 than in all of 2018. Connecticut, Ohio, and Oregon were among states that conducted detailed investigations; these 3 states identified 24 NDM-producing CRE isolates from 23 patients in period B. Overall, 5 (21.7%) of 22 patients with history available traveled internationally ≤12 months prior to culture; 17 (73.9%) acquired NDM-producing CRE domestically. Among 15 isolates sequenced, 8 (53.3%) carried NDM-5 (6 E. coli, 1 Enterobacter spp and 1 Klebsiella spp) and 7 (46.7%) carried NDM-1 (6 Enterobacter spp and 1 Klebsiella spp). Species were diverse; no single strain type was shared by >2 isolates. Conclusions: Detection of NDM-producing CRE has increased across the AR Lab Network. Among states with detailed information available, domestic acquisition was common, and no single variant or strain predominated. Aggressive public health response and further understanding of current US NDM-CRE epidemiology are needed to prevent further spread.
Disclosures: None
Funding: None
Identification of Colonized Patients During an Outbreak of Candida auris Using a Regional Health Information Exchange
- Richard Brooks, Elisabeth Vaeth, Heather Saunders, Tim Blood, Brittany Grace, David Blythe, Liore Klein, Jacqueline Reuben, Regan Trappler, Preetha Iyengar, Emily Blake, Sarah Lineberger, Rehab Abdelfattah, Kathleen Tully, Kaitlin Forsberg, Maroya Walters, Snigdha Vallabhaneni
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s255-s256
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: In June 2019, the Maryland Department of Health (MDH) was notified of a hospitalized patient with Candida auris bloodstream infection. The MDH initiated a contact investigation to identify additional patients with C. auris colonization. Many of the contacts had been discharged home from the hospital and were therefore not available for screening. Healthcare facilities in Maryland, Virginia, and Washington, DC, submit patient data to a regional health information exchange (HIE) called the Chesapeake Regional Information System for our Patients (CRISP). CRISP includes a notification system that alerts providers when flagged patients have healthcare encounters. We aimed to use this system to identify discharged C. auris contacts on their next inpatient encounter to rapidly screen them and to detect new cases. Methods:C. auris contacts were defined as patients located on an inpatient unit on the same day, receiving wound care from the same team, or having a procedure in the same operating room on the same day as the index patient or any patients subsequently identified as having C. auris infection or colonization detected either during the normal course of clinical care or through screening. Contacts who remained hospitalized were screened during inpatient point prevalence surveys (PPSs). Contacts discharged to postacute-care facilities were screened by facility staff. Contacts who had been discharged home were flagged in CRISP, and MDH staff received CRISP encounter alerts when these patients were readmitted. MDH staff then contacted the admitting facilities to recommend screening for C. auris. Axilla and groin swabs were collected and tested by rt-PCR at the Mid-Atlantic Regional Antibiotic Resistance Laboratory Network laboratory. Results: As of October 8, 2019, 4,017 contacts were identified. Among these, 936 (23%) contacts at 56 healthcare facilities (33 acute-care hospitals and 23 postacute-care facilities) were screened for C. auris, and 10 patients with C. auris colonization were identified (1.1% of contacts who underwent C. auris screening). Of these, 6 (60%) were identified through CRISP notification and 4 (40%) were identified by PPSs conducted in acute-care hospitals. Conclusions: In this ongoing C. auris outbreak, a large proportion of colonized patients was identified using an electronic encounter notification system within a regional HIE. This approach was effective for identifying opportunities to screen contacts at their next healthcare encounter and can augment other means of case detection, like PPSs. HIEs should incorporate mechanisms to facilitate contact tracing for public health investigations.
Funding: None
Disclosures: None
Characteristics Associated with Death in Patients with Carbapenem-Resistant Acinetobacter baumannii, United States, 2012–2017
- Hannah E. Reses, Kelly Hatfield, Jesse Jacob, Chris Bower, Elisabeth Vaeth, Jacquelyn Mounsey, Daniel Muleta, Medora Witwer, Ghinwa Dumyati, Emily Hancock, James Baggs, Maroya Walters, Sandra Bulens
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s59-s60
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Carbapenem-resistant Acinetobacter baumannii (CRAB) is an important cause of healthcare-associated infections with limited treatment options and high mortality. To describe risk factors for mortality, we evaluated characteristics associated with 30-day mortality in patients with CRAB identified through the Emerging Infections Program (EIP). Methods: From January 2012 through December 2017, 8 EIP sites (CO, GA, MD, MN, NM, NY, OR, TN) participated in active, laboratory-, and population-based surveillance for CRAB. An incident case was defined as patient’s first isolation in a 30-day period of A. baumannii complex from sterile sites or urine with resistance to ≥1 carbapenem (excluding ertapenem). Medical records were abstracted. Patients were matched to state vital records to assess mortality within 30 days of incident culture collection. We developed 2 multivariable logistic regression models (1 for sterile site cases and 1 for urine cases) to evaluate characteristics associated with 30-day mortality. Results: We identified 744 patients contributing 863 cases, of which 185 of 863 cases (21.4%) died within 30 days of culture, including 113 of 257 cases (44.0%) isolated from a sterile site and 72 of 606 cases (11.9%) isolated from urine. Among 628 hospitalized cases, death occurred in 159 cases (25.3%). Among hospitalized fatal cases, death occurred after hospital discharge in 27 of 57 urine cases (47.4%) and 21 of 102 cases from sterile sites (20.6%). Among sterile site cases, female sex, intensive care unit (ICU) stay after culture, location in a healthcare facility, including a long-term care facility (LTCF), 3 days before culture, and diagnosis of septic shock were associated with increased odds of death in the model (Fig. 1). In urine cases, age 40–54 or ≥75 years, ICU stay after culture, presence of an indwelling device other than a urinary catheter or central line (eg, endotracheal tube), location in a LTCF 3 days before culture, diagnosis of septic shock, and Charlson comorbidity score ≥3 were associated with increased odds of mortality (Fig. 2). Conclusion: Overall 30-day mortality was high among patients with CRAB, including patients with CRAB isolated from urine. A substantial fraction of mortality occurred after discharge, especially among patients with urine cases. Although there were some differences in characteristics associated with mortality in patients with CRAB isolated from sterile sites versus urine, LTCF exposure and severe illness were associated with mortality in both patient groups. CRAB was associated with major mortality in these patients with evidence of healthcare experience and complex illness. More work is needed to determine whether prevention of CRAB infections would improve outcomes.
Funding: None
Disclosures: None
Transmission of Carbapenemase-Producing Hypervirulent Klebsiella pneumoniae in Georgia, 2018–2019
- Jeanne Negley, Elizabeth Smith, Maroya Walters, Tonia Parrott, Richard Stanton, David Ham, Jacobs Slifka Kara, Patricia Kopp, Mary Connelly, Gebre Tiga, Gillian McAllister, Alison Halpin, Cherie Drenzek
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s414-s415
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: In April 2019, the Georgia Department of Public Health (DPH) initiated whole-genome sequencing (WGS) on NDM-producing Enterobacteriaceae identified since January 2018. The WGS data analyzed at CDC identified related Klebsiella pneumoniae isolates with hypervirulence markers from 2 patients. Carbapenemase-producing hypervirulent K. pneumoniae (CP-hvKP) are rarely reported in the United States, but they can to cause serious, highly resistant, invasive infections. We conducted an investigation to identify cases and prevent spread. Methods: We defined a case as NDM-producing K. pneumoniae with ≥4 hypervirulence markers identified by WGS, isolated from any specimen source from a Georgia patient. We reviewed the case patient’s medical history to identify potentially affected facilities. We also performed PCR-based colonization screening and retrospective and prospective laboratory-based surveillance. Finally, we assessed facility infection control practices. Results: Overall, 7 cases from 3 case patients (A, B, and C) were identified (Fig. 1). The index case specimen was collected from case-patient A at ventilator-capable skilled nursing facility 1 (vSNF1) in May 2018. Case-patient A had been hospitalized for 1 month in India before transfer to the United States. Case-patient B’s initial isolate was collected in January 2019 on admission to vSNF2 from a critical access hospital (CAH). The CAH laboratory retrospectively identified case-patient C, who overlapped with case-patient B at the CAH in October 2018. The CAH and the vSNF2 are geographically distant from vSNF1. Case-patients B and C had no known epidemiologic links to case-patient A. Colonization screening occurred at vSNF1 in May 2018, following detection of NDM-producing K. pneumoniae from case-patient A ∼1 year before determining that the isolate carried hypervirulence markers. Among 30 residents screened, 1 had NDM and several had other carbapenemases. Subsequent screening did not identify additional NDM. Colonization screening of 112 vSNF2 residents and 13 CAH patients in 2019 did not reveal additional case patients; case-patient B resided at vSNF2 at the time of screening and remained colonized. At all 3 facilities, the DPH assessed infection control practices, issued recommendations to resolve lapses, and monitored implementation. The DPH sequenced all 27 Georgia NDM–K. pneumoniae isolates identified since January 2018; all were different multilocus sequence types from the CP-hvKP isolates, and none possessed hypervirulence markers. Conclusions: We hypothesize that CP-hvKP was imported by a patient hospitalized in India and spread to 3 Georgia facilities in 2 distinct geographic regions through indirect patient transfers. Although a response to contain NDM at vSNF1 in 2018 likely limited CP-hvKP transmission, WGS identified hvKP and established the relatedness of isolates from distinct regions, thereby directing the DPH’s additional containment activities to halt transmission.
Funding: None
Disclosures: None
Evaluation of Patient Risk Factors for Carbapenemase-Producing Organism Colonization
- Carolyn Stover, Allison Chan, Snigdha Vallabhaneni, Allison Brown, Amelia Keaton, Alicia Shugart, Nychie Dotson, Sebastian Arenas, Marion Kainer, Maroya Walters
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s229-s230
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Carbapenemase-producing organisms (CPOs) are a growing antibiotic resistance threat. Colonization screening can be used to identify asymptomatically colonized individuals for implementation of transmission-based precautions. Identifying high-risk patients and settings to prioritize screening recommendations can preserve facility resources. To inform screening recommendations, we analyzed CPO admission screens and screening conducted on point-prevalence surveys (PPSs) performed through the Antibiotic Resistance Laboratory Network’s Southeast Regional Laboratory (SE AR Lab Network). Methods: During 2017–2019, the SE AR Lab Network collected data via a REDCap survey for a subset of CPO screens on a limited set of easily determined patient risk factors. Rectal swabs were collected and tested with the Cepheid Carba-R. Specimens collected within 2 days of admission were classified as admission screening and the remainder were classified as PPS. Index cases were excluded from analyses. Odd ratios (ORs) and 95% confidence intervals were calculated, and a value of 0.1 was used for cells with a value of zero. Results: In total, 520 screens were conducted, which included 366 admission screens at 2 facilities and 154 screens from 27 PPSs at 8 facilities. CPOs were detected in 14 (2.7%) screens, including in 10 (2.7%) admission screens and in 4 (2.6%) contacts during PPSs; carbapenemases detected were Klebsiella pneumoniae carbapenemase (KPC) (n = 12), New Delhi Metallo-β-lactamase (NDM) (n = 1) and Verona Integron-Encoded Metallo-β-lactamase (VIM) (n = 1). One long-term acute care hospital (LTACH) performed universal admission screening, which accounted for 96% of admission screens and all 10 CPOs detected by admission screening. Mechanical ventilation (OR, 5.0; 95% CI, 1.4–18.0) and the presence of a tracheostomy (OR, 5.4; 95% CI, 1.5–19.4) were associated with a positive admission screen. Moreover, 8 facilities conducted PPSs: 4 acute care hospitals, 2 long-term acute care hospitals, and 2 nursing homes. CPO prevalence in long-term acute care hospitals was 4.8% (2 of 42), 2.4% (1 of 41) in acute care hospitals, and 1.5% (1 of 69) in nursing homes. Requiring assistance with bathing (OR, 4.8; 95% CI, 1.6–8.0) and stool incontinence (OR, 16.6; 95% CI, 13.4–19.8) were associated with a positive screen on PPSs. All 7 roommates of known cases tested negative for CPO colonization. Conclusions: Findings suggest that patients with certain easily assessed characteristics, such as mechanical ventilation, tracheostomy, or stool incontinence or who require bathing assistance, may be associated with CPO positivity during screening. Further data collection and analysis of such risk factors may provide insight for the development of more targeted admission and contact screening strategies.
Funding: None
Disclosures: None
Trimethoprim-Sulfamethoxazole Resistance Patterns Among Methicillin-Resistant Staphylococcus aureus, 2012–2018
- D. Cal Ham, Lucy Fike, Tara Fulton, Nychie Dotson, Rebecca Perlmutter, Ericka Kalp, Joseph Lutgring, Amy Gargis, Alison Laufer-Halpin, Alexander Kallen, Maroya Walters
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, p. s418
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Trimethoprim-sulfamethoxazole is commonly used for the treatment of noninvasive methicillin-resistant Staphylococcus aureus (MRSA) infections. Following a report from 2 facilities of increased trimethoprim-sulfamethoxazole resistance among MRSA infections, we assessed changes in resistance nationally and by state. Methods: We reviewed antibiotic susceptibility testing (AST) data for trimethoprim-sulfamethoxazole among S. aureus isolates associated with surgical site infections (SSIs), central-line–associated bloodstream infections (CLABSIs), and catheter-associated urinary tract infections (CAUTIs) from acute-care hospitals reported to the NHSN Device and Procedure Module from 2012 to 2018. We compared the pooled mean percentage of isolates nonsusceptible to trimethoprim-sulfamethoxazole in 2012 and 2018, stratified by MRSA and methicillin-sensitive Staphylococcus aureus (MSSA). Among MRSA isolates, we compared the percentage nonsusceptible to trimethoprim-sulfamethoxazole by healthcare-associated infection (HAI) type and state in 2012 and 2018. States with ≥20 MRSA isolates with AST reported each year were included in the state-level analysis. Results: Overall, 36,587 MRSA isolates and 46,824 MSSA isolates were reported from 2012 to 2018. Moreover, >80% of MRSA and MSSA isolates had trimethoprim-sulfamethoxazole AST reported each year. Nationally, the percentage of trimethoprim-sulfamethoxazole nonsusceptible among MRSA isolates was 3.9% in 2012 compared to 6.5% in 2018 (P < .001), but it was unchanged among MSSA isolates during the same period (1.1% in 2012 vs 1.4% in 2018; P = .08). Among MRSA surgical site infections (SSIs), the proportion of trimethoprim-sulfamethoxazole nonsusceptible isolates was 3.1% in 2012 versus 6.1% in 2018 (P < .001) but did not change significantly for CLABSIs or CAUTIs (Fig. 1). Among the 32 states that met the inclusion criteria, there were no significant decreases, whereas 4 (12.5%) showed significant increases in the percentage of MRSA that were trimethoprim-sulfamethoxazole nonsusceptible in 2018 compared to 2012: New Jersey (2.4% in 2012 vs 19.3% in 2018; P <.001); Florida (9.1% in 2012 vs 22.4% in 2018; P < .001); Maryland (0.0% in 2012 vs 10.9% in 2018; P < .01); and Pennsylvania (1.7% in 2012 vs 6.5% in 2018; P < .001). Conclusions: Nationally, there was a modest but significant increase in the percentage of MRSA HAI isolates nonsusceptible to trimethoprim-sulfamethoxazole in 2018 compared to 2012; however, 3 of 4 states with significant increases in nonsusceptibility had substantial, potentially clinically relevant increases (>10%). Ongoing characterization of MRSA isolates from Florida and New Jersey may provide insight into the underlying cause of these shifting patterns in trimethoprim-sulfamethoxazole resistance among MRSA. Healthcare personnel should select appropriate antibiotic regimens based on local resistance patterns, should monitor patients for treatment failure, and should report changes in resistance to the appropriate public health department.
Funding: None
Disclosures: None
Regional Public Health Response to Emerging Carbapenamase-Producing Organisms in Central Florida, 2019
- Danielle A. Rankin, Justine M. Celli, Danielle L. Walden, Allison Chan, Albert Burks, Nicole Castro, Sasha Nelson, Marion A. Kainer, Alvina K. Chu, Nychie Q. Dotson, Maroya S. Walters
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, p. s50
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Detection of unusual carbapenemase-producing organisms (CPOs) in a healthcare facility may signify broader regional spread. During investigation of a VIM-producing Pseudomonas aeruginosa (VIM-CRPA) outbreak in a long-term acute-care hospital in central Florida, enhanced surveillance identified VIM-CRPA from multiple facilities, denoting potential regional emergence. We evaluated infection control and performed screening for CPOs in skilled nursing facilities (SNFs) across the region to identify potential CPO reservoirs and improve practices. Methods: All SNFs in 2 central Florida counties were offered a facility-wide point-prevalence survey (PPS) for CPOs and a nonregulatory infection control consultation. PPSs were conducted using a PCR-based screening method; specimens with a carbapenemase gene detected were cultured to identify the organisms. Infection control assessments focused on direct observations of hand hygiene (HH), environmental cleaning, and the sink splash zone. Thoroughness of environmental cleaning was evaluated using fluorescent markers applied to 6 standardized high-touch surfaces in at least 2 rooms per facility. Results: Overall, 21 (48%) SNFs in the 2-county region participated; 18 conducted PPS. Bed size ranged from 40 to 391, 5 (24%) facilities were ventilator-capable SNFs (vSNFs), and 12 had short-stay inpatient rehabilitation units. Of 1,338 residents approached, 649 agreed to rectal screening, and 14 (2.2%) carried CPOs. CPO-colonized residents were from the ventilator-capable units of 3 vSNFs (KPC-CRE=7; KPC-CRPA=1) and from short-stay units of 2 additional facilities (VIM-CRPA, n = 5; KPC-CRE, n = 1). Among the 5 facilities where CPO colonization was identified, the prevalence ranged from 1.1% in a short-stay unit to 16.1% in a ventilator unit. All facilities had access to soap and water in resident bathrooms; 14 (67%) had alcohol-based hand rubs accessible. Overall, mean facility HH adherence was 52% (range, 37%–66%; mean observations per facility = 106) (Fig. 1). We observed the use of non–EPA-registered disinfectants and cross contamination from dirty to clean areas during environmental cleaning; the overall surface cleaning rate was 46% (n = 178 rooms); only 1 room had all 6 markers removed. Resident supplies were frequently stored in the sink splash zone. Conclusions: A regional assessment conducted in response to emergence of VIM-CRPA identified a relatively low CPO prevalence at participating SNFs; CPOs were primarily identified in vSNFs and among short-stay residents. Across facilities, we observed low adherence to core infection control practices that could facilitate spread of CPOs and other resistant organisms. In this region, targeting ventilator and short-stay units of SNFs for surveillance and infection control efforts may have the greatest prevention impact.
Funding: None
Disclosures: None
Optimizing Sentinel Surveillance to Target Containment of Emerging Multidrug-Resistant Organisms in Regional Networks
- Prabasaj Paul, Rachel Slayton, Alexander Kallen, Maroya Walters, John Jernigan
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s336-s337
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Successful containment of regional outbreaks of emerging multidrug-resistant organisms (MDROs) relies on early outbreak detection. However, deploying regional containment is resource intensive; understanding the distribution of different types of outbreaks might aid in further classifying types of responses. Objective: We used a stochastic model of disease transmission in a region where healthcare facilities are linked by patient sharing to explore optimal strategies for early outbreak detection. Methods: We simulated the introduction and spread of Candida auris in a region using a lumped-parameter stochastic adaptation of a previously described deterministic model (Clin Infect Dis 2019 Mar 28. doi:10.1093/cid/ciz248). Stochasticity was incorporated to capture early-stage behavior of outbreaks with greater accuracy than was possible with a deterministic model. The model includes the real patient sharing network among healthcare facilities in an exemplary US state, using hospital claims data and the minimum data set from the CMS for 2015. Disease progression rates for C. auris were estimated from surveillance data and the literature. Each simulated outbreak was initiated with an importation to a Dartmouth Atlas of Health Care hospital referral region. To estimate the potential burden, we quantified the “facility-time” period during which infectious patients presented a risk of subsequent transmission within each healthcare facility. Results: Of the 28,000 simulated outbreaks initiated with an importation to the community, 2,534 resulted in patients entering the healthcare facility network. Among those, 2,480 (98%) initiated a short outbreak that died out or quickly attenuated within 2 years without additional intervention. In the simulations, if containment responses were initiated for each of those short outbreaks, facility time at risk decreased by only 3%. If containment responses were initiated for the 54 (2%) outbreaks lasting 2 years or longer, facility time at risk decreased by 79%. Sentinel surveillance through point-prevalence surveys (PPSs) at the 23 skilled-nursing facilities caring for ventilated patients (vSNF) in the network detected 50 (93%) of the 54 longer outbreaks (median, 235 days to detection). Quarterly PPSs at the 23 largest acute-care hospitals (ie, most discharges) detected 48 longer outbreaks (89%), but the time to detection was longer (median, 716 days to detection). Quarterly PPSs also identified 76 short-term outbreaks (in comparison to only 14 via vSNF PPS) that self-terminated without intervention. Conclusions: A vSNF-based sentinel surveillance system likely provides better information for guiding regional intervention for the containment of emerging MDROs than a similarly sized acute-care hospital–based system.
Funding: None
Disclosures: None







